Amongst peers and professionals: Learning from what we seek in online discussions of death and dying
In April and May 2021 we held a series of conversations about wellbeing and terminal illness. We brought together practitioners, academics and individuals to talk about what really matters to people with life-limiting or terminal illness, and how to develop support which puts their wellbeing – and that of their families – at the heart.
In the first of these entitled ‘conversations at the end of life’ – Ciaran Cummins, a researcher at the think-tank Demos, talked about how the use of online forums for support around death and dying, sheds light on integrating informal spaces into formal care.
For many, discussions about support at the end of life remain a taboo: conversations that we prefer to delay until we are forced to have them. Yet, for many others these topics are pervasive, be it for the bereaved or those who have, or care for those who have, a life-limiting illness.
Many in this position wish to discuss their experiences with others who have lived through the same, and online forums dedicated to grief, care and related topics have brought new possibilities for such connection. Our report seeks to understand this better, and finds that people turn to these spaces to:
- Seek comfort and validation from others going through similar experiences
- Build their own capabilities, by building their understanding and access to information about end of life
- Find a space where they can support others and be supported themselves.
These needs are well understood by practitioners, but, as they told us, this research sheds light on how these play out online and points to how user-led online support could be connected up with formal support.
Practitioners recognised how these forums have been particularly valuable in allowing people to have greater say over their support, not least those who find themselves marginalised from this elsewhere. From those with poor experiences of the care system, to those whose grief is misunderstood, these communities offer solidarity, companionship and information. To preserve dignity, end of life support should be centred around what an individual chooses as well as needs, and in this respect these accessible, user-led environments which provide for some what they cannot find elsewhere, have a demonstrable value. At the same time, and particularly for the most vulnerable who turn to these spaces, expert care is vital. Not only to ensure more complex needs are met, but also so that those who might be the targets of harmful online activity such as exploitation are safeguarded. This means integration of forums into health services is necessary, bringing greater oversight, presence of and support from health professionals. The danger is if this goes too far, undoing the very democratisation of support that users celebrate about these spaces.
This tension can be resolved through a new model, where the role of both formal and more user-led online support is clearly defined but with ongoing communication and collaboration between all.
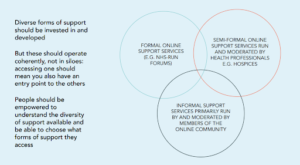
Under this model, logging into these forums would signpost you also to formal options, while someone looking for information from the NHS would also be given information about online communities. Neither replaces the other, rather they are complementary. This chimes with the NHS’ focus on ‘Connected digital systems’, and to build this connection we need a shared database, created by organisations providing support at the end of life, those providing online spaces and the NHS, to inform the kind of signposting described above.
We believe there is more we can learn about these spaces, but what we do know is they are providing an accessible kind of support where those affected can support one another as they wish. To paraphrase one user, “Our forum is like sitting down with a group of friends. We can gather, and open up to each other about what is in our hearts.”
Read the summary of our dying well conversations
Dying Well: Wellbeing at the end of life
